
Breast Reduction in Melbourne, Australia
Breast reduction surgery is a procedure that may help to reduce the size of and reshape the breasts, providing relief from physical discomfort and altering the overall aesthetic appearance.
Dr Craig Rubinstein, one of the experienced plastic surgeons based in Melbourne, offers breast reduction surgery to help women achieve the desired breast size. Dr Rubinstein understands the unique concerns and goals of each patient, providing personalised treatment plans to deliver optimal results.
DOWNLOAD GUIDE
Considering breast reduction surgery? Information is just one click away.

What is a Breast Reduction Surgery?
The aim of breast reduction surgery/Reduction Mammoplasty is to address the concerns and discomfort of larger, heavier breasts.
The symptoms of large, heavy breasts can vary from person to person, but common symptoms may include:
- Neck, shoulder, and back pain:
- Excessive weight and strain on the upper body can lead to chronic pain and discomfort in these areas.
- Poor posture:
- The weight of heavy breasts can pull the shoulders forward and contribute to a hunched posture.
- Skin irritation
- The skin underneath the breasts may become irritated, red, or develop rashes due to friction and moisture buildup.
- Grooves or indentations on the shoulders
- The bra straps digging into the shoulders can cause deep grooves or indentations.
- Limitations on physical activities
- Engaging in physical activities e.g. running, may be uncomfortable or difficult due to the weight and movement of the breasts.
- Emotional discomfort
- Some individuals may feel self-conscious or experience emotional distress due to the attention drawn to their breast size.
It’s important to note that each person’s experience is unique. Not all individuals with large breasts will experience the same symptoms.
Consult with a medical professional to discuss individual concerns and explore potential solutions.

What are the Potential Outcomes of Breast Reduction?
Breast reduction surgery, also known as reduction mammoplasty, offers several outcomes to individuals with large, heavy breasts:
Alleviation of physical discomfort
Breast reduction surgery may help relieve chronic pain and discomfort in the neck, shoulders, and back caused by the excessive weight of large breasts.
Addressed posture
Large, heavy breasts can contribute to poor posture, including rounded shoulders and a forward head position.
Breast reduction surgery may help alter posture by reducing the weight and volume of the breasts.
Relief from skin irritation and infections
Excessive breast size can lead to skin irritations, rashes, and infections in the areas underneath the breasts.
Breast reduction surgery works to eliminate the excess skin and tissue, reducing the friction and moisture buildup that contribute to these issues.
Increased physical activity
Engaging in physical activities and exercise can be challenging for individuals with large breasts.
Breast reduction surgery may enable individuals to participate in sports, fitness, and other physical activities more comfortably and easily.
Altered symmetry and proportions
Breast reduction surgery not only reduces the size and weight of the breasts but also changes their shape and position.
The procedure aims to create breasts that are more symmetrical and proportionate to the body.
It’s important to consult with a qualified plastic surgeon to discuss individual goals, expectations, and potential risks associated with breast reduction surgery.
Are You a Suitable Candidate?
Determining if you are a suitable candidate for breast reduction surgery involves a comprehensive evaluation with a qualified plastic surgeon. However, asking yourself these questions can provide a preliminary assessment of whether the procedure may be suitable:
- Do you experience discomfort or pain due to large, heavy breasts?
- Are your nipples enlarged or stretched?
- Do you suffer from neck, back pain, or posture issues related to the weight of your breasts?
- Do your breasts hinder your ability to participate in physical activities or exercise?
- Can you commit to following post-operative instructions for recovery?
- Do you have realistic expectations about the potential outcomes of surgery?
While these questions can provide a general indication, it is important to consult with a qualified plastic surgeon for a comprehensive evaluation and personalised recommendation.
They will assess your individual situation, examine your breast anatomy, discuss your concerns and goals, and provide professional advice based on their expertise. They will take into consideration factors such as your overall health, breast size and shape, skin elasticity, and any specific issues you may be experiencing.
A plastic surgeon will guide you through the process, explain the potential outcomes and risks, and help determine if you are a suitable candidate for breast reduction surgery.
Considering Breast Reduction Surgery? Get the Reduction Mammoplasty Guide!

Three Breast Reduction Surgical Techniques
There are three common techniques surgeons use for breast reduction procedures. The choice of technique depends on the expertise of the surgeon and your specific needs. Your surgeon will guide you in selecting the most suitable technique for your body and desired outcome.
Anchor Incision
Also known as a keyhole incision, the anchor incision is named due to its resemblance to the nautical anchor. The surgeon will make this incision under the areola and then down the centre of the breast similar to the LeJour technique. However, unlike the LeJour, the anchor incision has an additional/third, long incision along the inframammary crease.
Peri-Areolar Incision
The peri-areolar incision method has become slightly redundant over time. Many plastic surgeons consider the risks of this technique to outweigh the outcomes.
They often find alternative techniques that yield desired results with less risk to nipple function, sensation, and tissue integrity.
LeJour Incision or Lollipop Technique (Dr. Craig’s Preferred Method)
Dr. Craig Rubinstein prefers the LeJour incision, also known as the lollipop technique, for performing breast lifts and reductions. This technique provides significant lift, particularly for those with moderate ptosis. It involves removing a doughnut-shaped piece of tissue and making a straight incision down to the breast crease, resulting in a lollipop-shaped incision instead of an anchor-shaped one.
During your consultation with Dr Rubinstein, he will assess your unique situation and discuss the outcomes and considerations of each technique. Together, you can determine the most suitable approach to achieve your desired outcome.
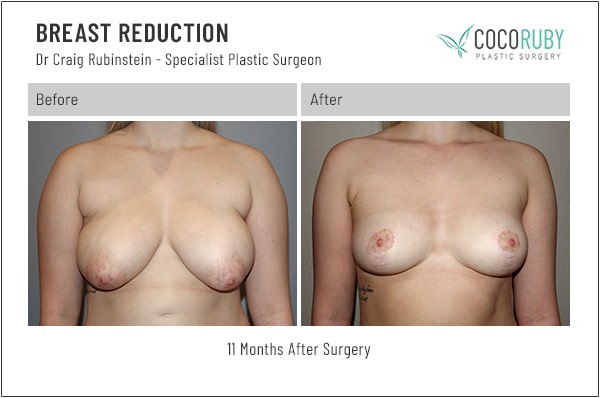
Breast Reduction Photos – Real Patient Before and After Gallery
Breast reduction (Reduction Mammoplasty) before and after photos from Dr Craig Rubinstein, Melbourne-based breast surgery plastic surgeon.
To see more Breast Reduction patient images, please contact us to book a consultation with Dr Craig Rubinstein or view more breast reductions of past patients.
Photo Disclaimer
The before and after photos displayed on our website or in our office are provided for informational purposes only. They are intended to offer an illustration of the potential outcomes that can be achieved through plastic and cosmetic surgery. However, it’s important to understand that individual results may vary, and the results of any surgical procedure cannot be guaranteed. The photos are not intended to serve as promises or a guarantee of specific results, but rather as a visual aid to help envision what is possible. It is crucial to recognise that each person is unique, and the outcome of surgery will be influenced by various factors such as overall health, body type, and healing ability. During your consultation, Dr. Rubinstein will carefully evaluate each individual and provide an honest and realistic assessment of what can be expected from the procedure.
The Breast Reduction Surgery – The Procedure
During a breast reduction procedure, the surgeon will remove excess breast tissue and redundant skin to achieve the desired size and shape. If required, the nipples may also be reshaped, repositioned, and lifted. In some cases, liposuction may also be used for removing fat from the torso and/or breasts.
The amount of breast tissue the surgeon will remove can vary significantly, ranging from 100g to as much as 5.5kg, depending on the individual’s needs.
A breast lift (mastopexy) is typically performed as part of the breast reduction procedure, if necessary. The duration of the surgery can range from 2 to 3 hours, depending on factors such as breast size, surgical technique, the surgeon’s expertise, and the collaborative efforts of the surgical team.
Breast Reduction – Reshaping of the Breast and Surrounding Areas with the Addition of Liposuction
During a breast reduction procedure, your surgeon may also use liposuction to reshape the breast and surrounding areas to achieve the desired contouring. This involves the removal of excess fat using a specialised suction technique.
Nipple and Areola Reshaping During Breast Reduction Surgery
During reduction mammoplasty, Dr Craig Rubinstein has the expertise to reshape/resize your areola/’nipples’ if they have become stretched or elongated.
He can reposition the nipples higher on the breasts. As an experienced plastic surgeon, Dr Rubinstein has the skill to reduce, reshape, and adjust the appearance of the areola and nipples during breast reduction surgery. This can result in smaller, rounder, and more proportionate-looking areolas. He utilises specialised instruments to achieve the requested aesthetic outcomes.
Does Breast Reduction Surgery Hurt?
Pain levels can vary from person to person, but it’s normal to experience some discomfort after breast reduction surgery. However, Dr Rubinstein will take measures to manage your pain and ensure you are as comfortable as possible during your recovery. This may include prescribing pain medications or recommending over-the-counter pain relievers. It’s important to follow your surgeon’s post-operative instructions, including taking any prescribed pain medications as directed. Over time, as your body heals, the discomfort will gradually subside. If you have concerns about pain management, it’s best to discuss them with your surgeon during your consultation or pre-operative appointments.
Will My Reduction Surgery Use Drains?
Dr Rubinstein prefers to perform drain-free breast reduction surgery whenever possible to ensure your comfort during the post-operative recovery period and minimise the risk of infection at drain insertion sites. However, in certain cases, drains may be necessary.
If Dr Rubinstein uses drains, he will remove them as soon as appropriate. The decision to use drains will depend on various factors, such as the extent of the surgery and individual patient needs.
Dr Rubinstein will discuss this with you and provide personalised recommendations based on your specific situation.
What is a ‘Lipo-Only’ Breast Reduction?
This is a liposuction-only breast reduction procedure. While it avoids the typical breast surgery scars, small scars may still be present at the sites where the liposuction cannulas are inserted.
It is crucial to understand that liposuction-only breast reduction is not the ideal choice for most patients. Although it may provide a minor reduction in breast size, it is limited in its ability to address issues such as excess skin and breast ptosis. In fact, it can potentially worsen these conditions by reducing breast tissue without addressing underlying concerns.
To determine the most suitable surgical approach for your specific needs, it is highly recommended to have a thorough discussion with a highly skilled plastic surgeon like Dr Craig Rubinstein. He can provide guidance and personalised recommendations based on your individual circumstances.
Recovery and Healing after Breast Reduction Surgery
The healing process after a breast reduction surgery can vary from patient to patient, with individual recovery times ranging from several weeks to a few months. On average, most patients can expect an initial recovery period of around 10-14 days if there are no complications or delays in healing. Adhering to all postoperative instructions provided by your surgeon is crucial for a smooth recovery.
Returning to work can typically occur after about 2 weeks, depending on the nature of your job. However, if your work involves heavy lifting or strenuous physical activity, it is important to wait until you have received clearance from your surgeon before resuming such tasks. Your surgeon will evaluate your progress and advise you on when it is safe to return to your regular work activities.

Exercise for Breast Reduction
After breast reduction surgery, it is important to follow your surgeon’s postoperative instructions regarding exercise. Generally, surgeons will advise patients to avoid rigorous activities and exercise for a certain period to allow for proper healing and recovery. Your surgeon will provide specific guidelines tailored to your individual case. It is important to gradually reintroduce exercise and listen to your body’s signals to avoid any strain or complications. Always consult with your surgeon before resuming any exercise routine after breast reduction surgery.
Rest is important
During surgery, your breast and surrounding tissues are disrupted. The healing period after breast reduction surgery is crucial and should not be rushed. Your body needs time to rest and recover from the surgical procedure. It is normal to experience bruising and swelling for a few days following the surgery. Each patient’s healing process and pain levels will vary. Over-the-counter pain medications are usually sufficient, but if necessary, your surgeon may prescribe additional painkillers to ensure your comfort and aid in sleep during the healing process. Dr Rubinstein utilises dissolvable stitches that do not require removal, minimising visible markings. However, it’s important to note that scarring will still occur. Our team will provide guidance on how to properly care for your incision lines as they heal.
After your breast reduction surgery, it is crucial to prioritise relaxation and avoid activities that can strain or stress your body. Refrain from stretching, pulling, heavy lifting, or engaging in strenuous exercise for at least six weeks. This allows your body to heal properly and reduces the risk of complications. Additionally, taking care of your skin is essential during the healing process. Follow the post-operative instructions provided by your surgeon, which may include gentle skincare routines and the use of appropriate support garments to provide adequate support and promote optimal healing.
How to Minimise Breast Reduction Scars
It is important to remember that all surgical procedures leave scars. However, Dr Rubinstein is cautious about scar placement and minimisation methods.
Dr Rubinstein’s dermal team also conducts follow-up treatments using special Lasers and Healite II to minimise your scars, with most scars being barely visible after 12 months.
Silicone strips and gels may also help minimise scars. We will arrange weekly appointments with our specialist nursing team after the procedure to ensure everything is healing well and to monitor your progress. You will see your surgeon and/or nurse and/or care team six to eight weeks later.
What is the Cost of a Breast Reduction?
The cost of breast reduction surgery can vary depending on several factors, including the surgeon’s experience and expertise, the complexity of the procedure, the surgical facility, and any additional treatments or services included. It is best to consult with a qualified plastic surgeon to get an accurate assessment of the cost specific to your individual needs and get a clear understanding of what is included in the total cost.
Additionally, some insurance plans may provide coverage for breast reduction surgery if it is deemed medically necessary, though you will still have out-of-pocket costs.
Breast Reduction on Medicare or Health Insurance
Some types of breast reduction surgery may be eligible for coverage by Medicare and Private Health Insurance. However, most reduction procedures are classified as cosmetic and will NOT be covered. Please discuss this with Dr Craig or your Patient Liaison for further information.
What are the Risks of Breast Reduction Surgery?
Breast reduction surgery, like any surgical procedure, carries certain risks and potential complications. It’s important to discuss these with your plastic surgeon before undergoing the procedure. Some possible risks and complications of breast reduction surgery include:
Poor Scarring
All surgical procedures result in some degree of scarring. Although your surgeon attempts to minimise the degree of scarring, you will have permanent scars.
The appearance of scars can vary between individuals, and some people will scar worse than others.
Infection
Infection is a potential risk with any surgery.
Antibiotics can usually treat the infection, but in some cases, additional procedures may be necessary.
Changes in nipple or breast sensation
Temporary or permanent changes in nipple or breast sensation may occur after breast reduction surgery.
This can range from increased sensitivity to decreased sensation or numbness in the nipples or breasts.
Changes in breast shape or size
While breast reduction aims to alter the shape and size of the breasts, there is a possibility of asymmetry, unevenness, or dissatisfaction with the final outcome.
Difficulty breastfeeding
Breast reduction surgery may affect the ability to breastfeed in some cases.
It’s important to discuss this with your surgeon if you have future plans for breastfeeding.
Delayed wound healing
In rare cases, the incisions may experience delayed wound healing, which can result in wound separation or poor scarring.
Blood clots
There is a small risk of developing blood clots in the legs (deep vein thrombosis) or the lungs (pulmonary embolism) after surgery.
Measures such as early mobilisation and the use of compression stockings are taken to minimise this risk.
Anesthesia risks
General anesthesia used during surgery carries its own set of risks, including adverse reactions to medications, breathing difficulties, and allergic reactions.
Unsatisfactory cosmetic results
While most patients are satisfied with the results of breast reduction surgery, there is a possibility of not achieving the desired cosmetic outcome.
It’s important to remember that these risks and complications are rare, and the majority of breast reduction surgeries are successful with minimal complications. Your surgeon will discuss these risks with you and take necessary precautions to minimize them.
Further Reading – Medical References
Visit the ASPS USA Plastic Surgeons Website for information about Breast Reduction Surgery
Better Health Website on Breast Surgery to reduce large breasts
Breast Reduction Melbourne by Coco Ruby Plastic Surgeons
Best Blogs on Breast Reduction
Top Trends on Breast Reduction Surgery
About Dr Craig Rubinstein
MED0001124843

Dr Craig Rubinstein FRACS (Fellow of the Royal Australasian College of Surgeons) is an experienced Melbourne Specialist Plastic Surgeon for breast and abdominoplasty surgery.
Dr Rubinstein offers women personalised abdominoplasty surgery and all forms of cosmetic breast surgery.
BOOK A CONSULTATION (03) 8849 1400
Next Steps in Your Surgical Journey

Want more information about your Procedure?
- Download a Free Procedure Guide on your chosen surgery.
- Visit the FAQs and read patient reviews to learn more about your intended procedure.
- For more information about pricing visit our cost page.
- You can also talk to our Patient Care Team from 9 to 5 pm Monday to Friday on (03) 8849 1400

About Your First Consultation
- Dr Rubinstein’s Consultation fee is $300.
- A referral from your GP or specialist is essential.
- A referral helps when claiming Medicare or Private Health Insurance coverage.
- Please contact the Patient Care Team at Coco Ruby Plastic Surgery to book your consultation.

What to Bring to Your Consultation
- You are more than welcome to bring a friend or relative to help discuss the information and your choices.
- Ensure you also take a lot of notes and thoroughly examine the documents provided.
- Please be aware you may need to undress for a physical exam so wear simple clothes.


